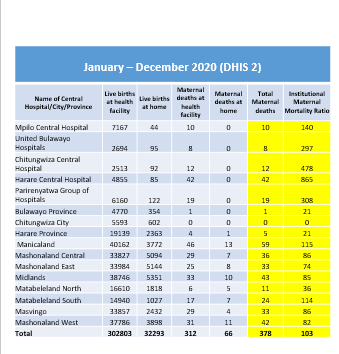
A total of 378 maternal deaths were reported between January and December 2020 in Zimbabwe, according to recent data released by the Ministry of Health and Child Care. 66 deaths occurred at home while 312 at health facilities and this shows that maternal mortality is still one of the major health concerns in Zimbabwe.
The World Health Organisation (WHO) defines maternal deaths as the annual number of female deaths from any cause related to or aggravated by pregnancy or its management but not from accidental or incidental causes during pregnancy and childbirth or within 42 days of termination of pregnancy, irrespective of the duration and site of pregnancy, expressed per 100 000 live births for a specified time.
In Sub-Saharan African countries alone, 196 000 cases of maternal deaths were reported between 2000 and 2017, accounting for roughly two-thirds of the global mortality rate. However, reports indicate that Maternal Mortality Ratio in Zimbabwe is declining as it went down from 614 in 2014 to 462 in 2019.
The total maternal deaths reported in Zimbabwe between January and December 2020 translate to a maternal mortality ratio of about 127 per 100 000 births. A Maternal Mortality Ratio of less than 100 is considered as low, between 100 and 299 as moderately low, and high when it is 300 to 499.
The top 5 causes of maternal deaths noted by the ministry include: bleeding after giving birth (26%), hypertensive diseases (16%) (high blood pressure which leads to violent fits during pregnancy), puerperal sepsis (10%) – fever & pain due to infection of the genital tract of a woman that occurs from the breaking of the waters (rapture of the membrane) or labour up to 42 days after giving birth, and post and peri abortal sepsis (9%) – serious infection of the uterus (fever & pain) due to induced abortion and C-section (5%).
There have been reports of increased teenage pregnancies in Zimbabwe. This has been worsened by Covid-19 induced school closures. One in three girls gets pregnant before the age of 18 and girls below the age of 19 account for 15 percent of the maternal mortality rate. Statistics also indicate that the national teenage pregnancy rate is at 22 percent.
The trend in teenage pregnancies is a challenge that should be addressed if Zimbabwe is to reduce maternal mortality rates as WHO states that the risk of maternal mortality is highest for adolescent girls below the age of 15 years.
On a positive note, certain measures have been adopted by the government to reduce maternal mortality. Reporting and auditing of all maternal deaths, and clinical mentorship for nurses and doctors at provincial and district levels have been rolled out.
The measures also include on-the-job training of nurses and doctors at all levels on Emergency Obstetric and Neonatal Care, utilization of the maternity waiting homes by pregnant mothers, implementation of new Ante-Natal Care (ANC) guidelines, procurement of essential maternal health equipment, drugs and consumables, and improved family planning services and training of service providers on the WHO 9 Standards on youth friendly service provision.
At the global level, Sustainable Development Goal (SDG) 3 of the WHO targets reducing the global Maternal Mortality Ratio to less than 70 per 100 000 live births by 2030. Zimbabwe should complement global efforts for the attainment of the goal to significantly reduce preventable maternal mortality.
There is a need for tailored strategies to address inequalities related to access to health care services between rural people and urban people.
Rural people still travel long distances to access medical services and this could be one of the reasons for giving birth at home. Some cultural and religious practices which discourage people from accessing medical services should also be addressed.
Highlights of the 2021 national budget indicate that the health sector has been allocated ZWL 54.7 billion which is 13% of the budget and higher than last year’s 10%.
However, this is still below the Abuja Declaration’s 15% threshold. Responsible authorities should also address the needs of health workers to prevent industrial action which can cripple health services delivery systems.
In June this year, health workers in Zimbabwe declared incapacitation only to call off the industrial action in September after an agreement with the Minister of Health and Child Care.
The declared incapacitation worsened difficulties in accessing health care services for the general public. WHO’s SDG 3 on maternal mortality can be attained if health care systems are improved.
– Justin Salani
[ssba-buttons]
magnificent put up, very informative. I’m wondering why the opposite experts of
this sector do not realize this. You should proceed your
writing. I am sure, you’ve a great readers’ base already!